For a diabetic patient, developing a foot ulcer can be one of the most serious complications. The nature of diabetes puts these individuals at higher risk for wounds on their lower extremities such as ulcers. Approximately 15% of diabetics cases have been known to result in ulcer development. And about 6% of diabetic patients with ulcers are admitted into the hospital for ulcer infection and complications.
But diabetics who take the time to understand and properly treat the side effects of their disease can minimize the risks and through preventative measures, some diabetics may even eliminate the need for diabetic foot ulcer treatment in the first place. Our podiatrists in Baltimore would like to help you learn. Let’s start with what exactly is an ulcer.
What is a Diabetic Foot Ulcer
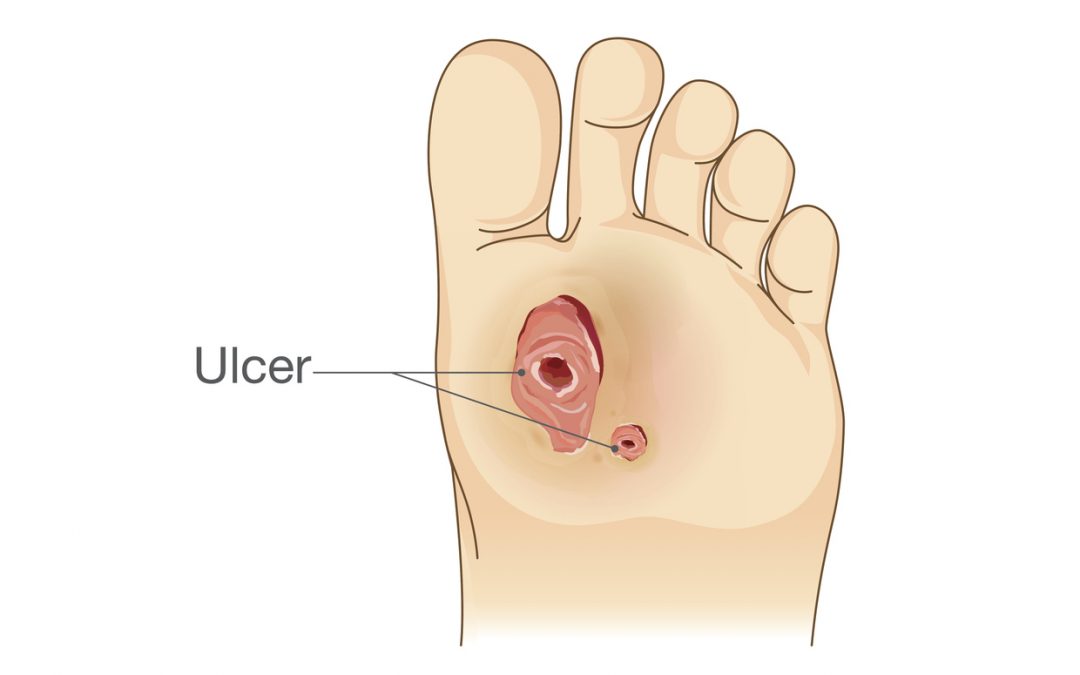
A foot ulcer is an open sore or wound usually located on the bottom of the foot and sometimes on the ankle or leg. A foot ulcer can either be on the surface of the skin or extend pretty deep through all three core layers of the skin.
How Does a Diabetic Foot Ulcer Develop?
The cause of foot ulcers is typically related to high blood glucose levels, which results in poor circulation of the feet, ankles, and even legs. Any cuts or sores that develop on a diabetic’s lower extremities are very slow to heal due to the lack of proper blood circulation, which increases the danger of infection. If proper diabetic foot ulcer treatment isn’t begun on time, the infection could lead to an onset up gangrene and potential amputation of the foot or limb.
A Foot Ulcer Can Lead to What Types of Infections?
If the foot ulcer is not properly treated and infection sets in, it can take the form of the following:
- A foot abscess or pocket of pus
- Gangrene (condition when body tissue darkens and dies – can lead to amputation)
- Cellulitis (bacterial skin infection that looks very swollen and red and spreads easily)
- Osteomyelitis (or bone infection)
How Can a Foot Ulcer Develop Unnoticed?
Foot ulcers can often develop undetected because most diabetics also have a nerve damage condition called neuropathy. This means that they have a hard time sensing or cannot sense heat, cold, pain or pressure at all. If they develop a small sore or cut and can’t sense that it’s even there, then the open wound will worsen and even get infected without immediate notice. That’s why it’s important for diabetics to follow best prevention practices or schedule immediate wound care treatment with our podiatrists in Baltimore if their feet already show signs of developing foot ulcers.
How to Prevent Diabetic Foot Ulcers
There are many preventative measures that you can take to minimize the chance of a diabetic foot ulcer and the need for wound care treatment. Among these are daily foot inspections, keeping your feet clean and dry, and many other simple but important tasks. Please reference this resource that our podiatrists in Baltimore put together for your convenience: Podiatrist Approved Tips for Diabetic Foot Care Health.
If you need professional diabetic foot ulcer treatment in Baltimore or wound care treatment in Baltimore and the surrounding areas or have any questions about the treatments described above, check out our Podiatry Associates locations and find a podiatrist near you. Feel free to call our scheduling office to discuss your specific situation: (833) 500-FEET.
Time to See a Podiatrist?
If you have any of the issues described above, it’s time to consult an expert. Connect with Podiatry Associates for an evaluation. All of our doctors are board certified/qualified and we’re dedicated to preserving your foot health.
Other Related Articles:
- What is the Impact of Diabetes in Wound Healing?
- The Key Role of a Podiatrist in Diabetic Foot Care
- 9 Healthy Tips for Diabetic Foot Care
- What is Diabetic Foot Pain?
- What Diabetic Foot Care Treatments Are Best Left to Your Podiatrist?
- Can a Podiatrist Perform Surgery? What Types?
- When to See A Podiatrist
- Everything You Need to Know About a Podiatrist
- 11 Things Every Patient Should Know About Foot Surgery